The Complete Breakdown Of PALS Algorithms Training And Why It Matters For Clinicians

Updated on: April 13, 2026
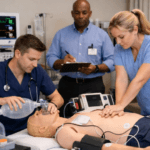
Pediatric emergencies require immediate and systematic intervention. Although evidence-based algorithms guide healthcare providers through complex, high-pressure situations involving children, the report from the American Heart Association on pediatric cardiac arrest survival rates remains concerning. Only 7.4 percent of children under one year survive to hospital discharge after out-of-hospital cardiac arrest. This statistic underscores the importance of PALS algorithms training for healthcare providers who manage pediatric emergencies.
Unlike adult resuscitation, pediatric emergencies are often caused by respiratory failure or shock rather than primary cardiac events. This necessitates specialized knowledge and systematic approaches. PALS algorithms training teaches you step-by-step protocols for recognizing and treating infants and children effectively.
So what exactly will you learn from PALS training? Keep scrolling to explore the essential algorithms used in pediatric emergencies.
Read More: PALS Algorithms Explained: Step-by-Step Guide for Beginners
What is the PALS Algorithm?
PALS algorithms are evidence-based, systematic protocols developed by the American Heart Association for managing pediatric emergencies. They provide clear, sequential steps for assessing and treating life-threatening conditions. Each algorithm addresses a specific emergency, including bradycardia, tachycardia, cardiac arrest, respiratory distress, and shock.
Read More: Decoding the purpose of the PALS certification course
A Complete Breakdown of PALS Algorithms
To learn the pediatric advanced life support algorithms, you need to understand how they connect. Each algorithm serves its own purpose, yet they share common assessment principles. Below is a breakdown of the core PALS algorithms:
Primary Assessment: The ABCDE Method
Before applying any algorithm, you must perform a proper assessment. The primary assessment helps you identify deterioration early, often before cardiac arrest occurs. The evaluation follows a structured sequence:
- Airway: Check for patency and obstruction. Determine whether the child can maintain their airway.
- Breathing: Assess respiratory rate, effort, and effectiveness. Listen for abnormal sounds and observe chest movement.
- Circulation: Evaluate heart rate, pulse quality, and perfusion. Capillary refill under two seconds indicates adequate perfusion.
- Disability: Determine neurological status using the AVPU scale (Alert, Voice, Pain, Unresponsive) or the pediatric Glasgow Coma Scale.
- Exposure: Look for trauma, rashes, or other physical findings while maintaining temperature control.
When a child has no pulse, this algorithm becomes your main guide. The approach differs based on whether the rhythm is shockable (ventricular fibrillation or pulseless ventricular tachycardia) or non-shockable (asystole or pulseless electrical activity).
- Verify cardiac arrest by checking the pulse within 10 seconds
- Begin high-quality CPR (Cardiopulmonary Resuscitation) immediately using a 15:2 compression-to-ventilation ratio for two rescuers
- Attach the monitor or defibrillator to identify the rhythm quickly
- For shockable rhythms, deliver a 2–4 J/kg shock and resume CPR right away
- Administer epinephrine 0.01 mg/kg every 3–5 minutes for all rhythms
- For persistent ventricular fibrillation, consider an amiodarone 5 mg/kg bolus
- Search for and treat reversible causes using the H’s and T’s mnemonic
- Reassess the rhythm every 2 minutes and continue CPR between interventions
Bradycardia with poor perfusion requires immediate intervention. A heart rate below 60 beats per minute with signs of inadequate systemic perfusion demands action. The steps for bradycardia management are:
- Identify symptomatic bradycardia: heart rate less than 60/min with poor perfusion
- Support airway management, breathing, and circulation with 100 percent oxygen
- Establish IV or IO access for medication administration
- Start CPR if the heart rate remains below 60/min despite oxygenation
- Administer epinephrine 0.01 mg/kg IV (Intravenous) /IO (Intraosseous) every 3–5 minutes
- Consider atropine 0.02 mg/kg for increased vagal tone or AV block
- Prepare for transcutaneous pacing if medications fail
- Treat underlying causes such as hypoxia, hypothermia, or heart block
Tachycardia algorithms differentiate between adequate and inadequate perfusion. You must also determine whether the QRS complex is narrow or wide. These distinctions guide the treatment pathway.
Steps for tachycardia with adequate perfusion:
- Identify tachycardia exceeding normal limits for age
- Assess perfusion status: capillary refill, mental status, and blood pressure
- Determine QRS width: narrow (less than 0.09 seconds) or wide
- For narrow-complex tachycardia, attempt vagal maneuvers first
- Administer adenosine 0.1 mg/kg rapid IV push (maximum 6 mg for the first dose)
- If needed, give a second adenosine dose of 0.2 mg/kg (maximum 12 mg)
- For wide-complex tachycardia, seek expert consultation immediately
- Prepare for synchronized cardioversion if the patient becomes unstable
Steps for tachycardia with poor perfusion:
- Recognize signs of shock: altered mental status, weak pulses, hypotension
- Provide immediate synchronized cardioversion at 0.5–1 J/kg
- Sedate the patient if conscious before cardioversion
- Increase energy to 2 J/kg if the first attempt is unsuccessful
- Establish IV/IO access and administer medications after cardioversion
- Consider amiodarone 5 mg/kg over 20–60 minutes for persistent rhythms
PALS Respiratory Distress and Failure Algorithm
Respiratory emergencies are the most common cause of pediatric cardiac arrest. This algorithm categorizes problems into upper airway obstruction, lower airway obstruction, lung tissue disease, and disordered control of breathing.
Steps for respiratory emergency management:
- Assess work of breathing: retractions, grunting, nasal flaring
- Identify the specific respiratory problem category through clinical signs
- Position the patient to optimize airway patency
- Provide supplemental oxygen with a target SpO₂ of 94 percent or higher
- For upper airway obstruction, allow the position of comfort and avoid agitation
- For lower airway obstruction, administer bronchodilators and consider steroids
- Support ventilation with a bag-mask if respiratory failure develops
- Prepare for an advanced airway if the patient cannot maintain oxygenation
Shock management requires rapid fluid resuscitation and early identification of the shock type. Pediatric patients can maintain normal blood pressure until they have lost a significant amount of circulating volume. The algorithm for shock management includes:
- Recognize shock: tachycardia, weak pulses, delayed capillary refill, altered mental status
- Establish vascular access (IV or IO) immediately
- Administer a 20 mL/kg isotonic crystalloid bolus rapidly
- Reassess perfusion after each bolus
- Repeat fluid boluses up to 60 mL/kg total in the first hour
- Identify shock type: hypovolemic, distributive, cardiogenic, or obstructive
- For distributive shock (sepsis), consider early vasopressors
- Monitor for fluid overload: hepatomegaly, crackles, and increased work of breathing
Read More: Identifying and Treating Pulseless Ventricular Tachycardia
How PALS Algorithm Training Benefits Clinicians
PALS algorithms course builds confidence that extends beyond pediatric units. You learn pattern recognition that saves crucial seconds during emergencies. Here is how it benefits clinicians:
Enhanced Decision-Making Speed
When cardiac arrest occurs, there is no time for uncertainty. PALS algorithms training creates mental frameworks that accelerate your response. Research from the Get With The Guidelines-Resuscitation registry shows that survival rates improved to 43 percent over a decade with systematic approaches.
Improved Team Coordination
Pediatric resuscitations require seamless teamwork. The PALS algorithm certification teaches you defined roles and closed-loop communication. Everyone communicates using the same clinical language. Effective team dynamics directly correlate with better patient outcomes.
Reduced Medical Errors
Algorithms minimize the risk of critical omissions during high-stress situations. The structured approach keeps you on track when stress is high. Algorithm-based care reduces medication errors by standardizing weight-based dosing.
What are the Challenges in PALS Algorithm Training?
The complexity and volume of PALS algorithms can be overwhelming during high-pressure situations. Here are the key challenges and solutions.
Information Overload and Complexity
PALS algorithms contain numerous decision trees with age-specific variables. You must remember different compression depths, ventilation rates, and energy doses for each patient population.
Solutions:
- Break algorithms into smaller, manageable sections for study
- Focus on one algorithm at a time instead of learning all at once
- Use spaced repetition techniques to improve long-term retention
Infrequent Use in Clinical Practice
Most healthcare providers rarely encounter pediatric arrests during daily practice. Without frequent exposure, your skills and knowledge naturally fade.
Solutions:
- Participate in quarterly simulation scenarios with your team
- Review algorithms monthly during downtime in your department
- Join online communities that discuss pediatric emergency cases
Medication Dose Calculations Under Pressure
Weight-based dosing adds complexity during emergencies when every second counts. You must calculate epinephrine, amiodarone, and fluid boluses accurately while performing other critical tasks.
Solutions:
- Use length-based resuscitation tapes for immediate weight estimation
- Keep pre-calculated dose cards readily available in pediatric areas
- Practice dose calculations regularly during non-emergency situations
Differentiating Between Similar Algorithms
Tachycardia and bradycardia algorithms share some treatment components but require distinct approaches. The pressure of a real emergency can exacerbate confusion between similar pathways.
Solutions:
- Study algorithms side by side to understand their distinct differences
- Create comparison charts that highlight unique features of each algorithm
- Use scenario-based learning that requires selecting the correct algorithm
PALS Algorithm Training: Handle Pediatric Emergencies with Confidence
PALS algorithm training provides you with proven protocols for dealing with pediatric emergencies. Learning PALS algorithms is more than just getting certified; it ensures you’re ready when a child’s life depends on your actions. Although the algorithms may appear complex at first, with consistent practice and the appropriate training approach, they become second nature.
If you are a busy clinician with demanding schedules, the online PALS course may be an excellent choice. Learn at your own pace, review difficult concepts whenever necessary, and complete certification requirements without interfering with your clinical responsibilities.
FAQs
1. Can I take PALS certification online?
Yes. Online PALS certification is available from accredited providers. The American Heart Association offers online learning, but be sure to verify employer acceptance. Most facilities accept online certification if it meets AHA or comparable international standards.
2. What equipment do I need for PALS algorithms?
Essential equipment for implementing PALS algorithms effectively includes:
- Pediatric bag-mask devices in multiple sizes (infant, child, adolescent)
- Appropriately sized oropharyngeal and nasopharyngeal airways
- Intravenous (IV) and intraosseous (IO) access supplies
- Defibrillators with pediatric pads and energy settings
- Emergency medications with pre-calculated dosing charts
- Length-based resuscitation tapes for quick weight estimation
3. What happens if I fail the PALS exam?
If you do not pass the written exam or skills testing on your first attempt, instructors typically provide remediation and retesting opportunities. You will review areas of weakness with the instructor, then retake the portion you did not pass. Most training centers allow at least one retake on the same day at no additional cost.
PALS CERTIFICATION
Author
PALS Certification is a trusted provider of online life support training, offering PALS, BLS, and ACLS certification and renewal courses. Our flexible training programs follow industry guidelines, offer self-paced learning and instant certification, ensuring providers stay compliant, advance their credentials, and deliver high-quality patient care.