- 4.0 CE Credit Hours
- For Pediatric Responders
- Includes Videos, Megacode Scenarios, Practice Tests & More
- FREE BLS Included
$119.00 $169.00
Get CertificateThe PALS (Pediatric Advanced Life Support) Tachycardia Initial Management Algorithm provides a systematic approach for healthcare providers to assess and manage pediatric patients with tachycardia. It involves evaluating the patient’s clinical condition, determining the presence of signs of poor perfusion, and categorizing the tachycardia as narrow or wide complex.
Based on the assessment findings, interventions such as vagal maneuvers, adenosine administration, synchronized cardioversion, or expert consultation may be recommended to stabilize the patient and restore normal heart rhythm. The below algorithm ensures timely and appropriate management of pediatric tachycardia to optimize patient outcomes.

$199.00

| Age Group | Normal Heart Rate (bpm) |
| Newborns (0 to 1 month) | 70 to 190 beats per minute (bpm) |
| Infants (1 to 12 months) | 80 to 160 bpm |
| Toddlers (1 to 3 years) | 80 to 130 bpm |
| Preschoolers (3 to 5 years) | 80 to 120 bpm |
| School-age children (6 to 12 years) | 70 to 110 bpm |
| Adolescents (13 to 18 years) | 60 to 100 bpm |
$119.00 $169.00
Get Certificate$119.00 $169.00
Get Certificate$36.95 $39.90
Get Certificate
The PALS Bradycardia Algorithm is a systematic approach for managing slow heart rates in pediatric patients.
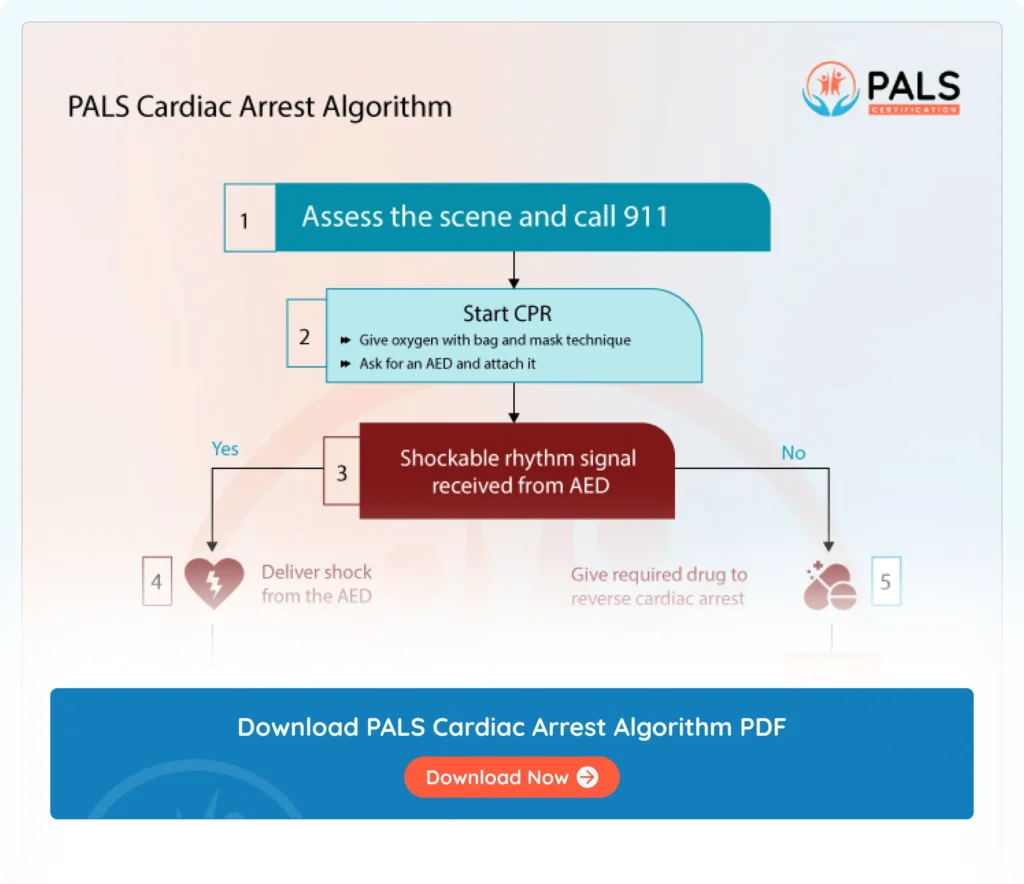
The PALS (Pediatric Advanced Life Support) algorithm is a standardized set of guidelines used in emergency medicine to manage pediatric cardiac arrest situations.

PALS Post Arrest Shock Management Algorithm outlines steps after ROSC for pediatric patients emphasizing critical interventions for stabilization