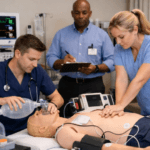
PALS for Prehospital vs In-Hospital Settings: Challenges & Solutions
Updated on: December 26, 2025
Pediatric emergencies are crucial across all settings. According to the Sudden Cardiac Arrest Foundation, almost 16% of children aged 1 to 18 who had an out-of-hospital cardiac arrest in 2023 survived until hospital discharge. The survival rate depends greatly on how quickly and effectively life support interventions are initiated. Pediatric Advanced Life Support (PALS) allows healthcare professionals to recognize and respond to these critical scenarios. However, there are key differences between prehospital EMS and in-hospital care environments, as well as in how PALS is applied in both settings.
In this guide, we will discuss the goals of PALS and the differences between EMS staff vs hospital teams. This will also help you learn how to restore oxygenation, circulation, and life.
Read More: What are the causes of cardiac arrest in a pregnant patient?
How Does PALS Work Across Prehospital vs In-Hospital Settings?
PALS usually begins at the scene of an emergency, such as your home, school, or a stadium, in prehospital environments. In most cases, EMS professionals are the first to analyze and initiate advanced life-saving interventions to save the pediatric victims.
That’s because their training focuses on rapid assessment with the help of the Pediatric Assessment Triangle (PAT), effective airway management, immediate cardiopulmonary resuscitation (CPR), and prompt defibrillation.
Conversely, hospital teams often operate in a controlled environment with diagnostic tools, multidisciplinary support, and specialized pediatric equipment. Physicians, nurses, and respiratory therapists often collaborate to assist pediatric patients in in-hospital settings. Activities like the early recognition of deterioration, advanced interventions, and medication administration are key parts of this process.
Differences Between EMS Staff vs Hospital Teams
As mentioned, PALS always works differently across prehospital and in-hospital settings. If you are interested in this field, you must know the key differences between EMS staff vs hospital teams. Here’s an overview:
| Category |
EMS Staff (Prehospital) |
Hospital Teams (In-Hospital) |
| Objective |
Ensure that the patient reaches the hospital safely. |
Provide advanced treatment and care to emergency pediatric patients. |
| Environment |
Unpredictable locations like homes, public spaces, or ambulances |
Controlled environment with access to equipment, specialists, and support staff. |
| Team Composition |
Paramedics, EMTs, and sometimes flight nurses. |
Pediatricians, emergency physicians, nurses, respiratory therapists, and specialists. |
| Available Equipment |
Often depends on portable monitors, defibrillators, airway kits, and medications. |
Access to full resuscitation carts, ventilators, lab tests, and imaging. |
| PALS Focus |
Rapid assessment, airway stabilization, CPR initiation, and transport coordination. |
Continuous monitoring, advanced interventions, and post-resuscitation management. |
| Communication |
Often depends on radio or telemedicine coordination with hospital teams. |
Direct communication and collaboration within the hospital team. |
| Challenges |
Limited resources, environmental constraints, and time-sensitive decisions. |
Multiple specialists, communication gap, and the burden of ensuring proper handoffs. |
Read More: 4 Levels of EMT Certification: EMR, EMT, AEMT & Paramedic
Differences Between EMS Staff vs Hospital Teams in PALS
| Category |
EMS Staff (Prehospital) |
Hospital Teams (In-Hospital) |
| Objective |
Safe transport to the hospital |
Advanced pediatric emergency care |
| Environment |
Unpredictable, mobile settings |
Controlled, well-equipped setup |
| Team |
Paramedics, EMTs, flight nurses |
Doctors, nurses, specialists |
| Equipment |
Portable kits, defibrillators |
Full resus cart, labs, imaging |
| PALS Focus |
Airway, CPR, rapid transport |
Continuous monitoring, interventions |
| Communication |
Radio or telemedicine links |
Direct in-team coordination |
| Challenges |
Limited tools, time pressure |
Coordination gaps, complex systems |
What are the Challenges of Applying PALS in Prehospital Settings?
Healthcare professionals can easily apply PALS across all prehospital settings. However, they may face a few hassles during this process, which are quite preventable, too. Here’s an overview of these limitations.
Environmental Limitations
Saving the lives of children or infants may become difficult if you are exposed to confined spaces, poor lighting, weather conditions, or noisy crowds. Airway management or chest compressions on uneven ground can also compromise the quality of CPR in medical emergencies.
Resource and Personnel Constraints
EMS teams usually have one or two paramedics, which may limit their ability to perform simultaneous interventions. This is unlike hospitals, where one provider manages the airway while another administers medications. That is why prehospital PALS often requires multitasking under extreme pressure.
Limited Access to Pediatric Expertise
Hospital staff can quickly consult pediatricians or specialists when necessary, but EMS providers usually operate without such support. Their decisions on medication, defibrillation, or airway interventions depend entirely on field training and protocol familiarity. This can also lead to stress and uncertainty in traumatic situations.
Documentation and Continuity of Care
Accurate documentation during prehospital resuscitation can be difficult. However, it is mandatory for hospital teams to understand what interventions have already been performed. Any issue with the transfer of information can easily lead to redundancy or omission of key steps after the patient is shifted to the hospital.
What are the Challenges of Applying PALS in In-Hospital Settings?
Even well-equipped hospitals face multiple challenges when implementing PALS treatments. These limitations may arise from system coordination or the complexities of multidisciplinary response teams. The primary ones include:
Team Coordination and Communication
A hospital team may include multiple members, such as pediatricians, anesthesiologists, nurses, respiratory therapists, and pharmacists. This diversity of roles can often lead to communication breakdowns, role confusion, or delays in the long run.
Time-Critical Decision-Making
Hospital staff can always access advanced tools and diagnostics during emergencies. However, delays in recognizing early signs of respiratory distress or shock can result in health deterioration of patients. The primary challenge in this case is to maintain situational awareness in case there are any busy emergency departments or ICUs.
Equipment and Resource Availability
Most hospitals generally have superior resources. However, the availability of correctly sized pediatric equipment or pre-prepared medication doses can still be a barrier. Sometimes, your resuscitation efforts may also slow down because of incorrect defibrillator settings or lack of immediate vascular access tools.
Training Consistency and Skill Retention
Every staff member cannot participate regularly in pediatric resuscitation, especially in general or adult-focused hospitals. This limited exposure can lead to a deterioration of skills in the long run. This further makes PALS certification renewals and simulation-based refreshers mandatory to maintain competence and confidence.
Documentation and Data Integration
Accurate, real-time documentation is the key to ensuring patient safety and well-being. Even with electronic medical records (EMRs), inputting key signs, medication doses, and timestamps while performing critical interventions can be difficult. Post-event data analysis is the main key to quality improvement but it depends heavily on consistent, detailed documentation.
Read More: One & Two Rescuer BLS for Infants (0 to 12 Months Old)
What are the Solutions to Bridge Gaps in PALS?
The positive part about working as a PALS-certified expert is that you can follow several strategies to overcome the challenges discussed above. Here are some key strategies that can help bridge the gaps in PALS:
Strengthen Communication and Leadership
Clear leadership and structured communication are the keys to ensuring effective PALS leadership. Both EMS and hospital teams benefit from adopting closed-loop communication, where commands are clearly given, acknowledged, and confirmed. Most importantly, leadership roles must be assigned at the start of any resuscitation to improve team performance.
Standardize Protocols Across Prehospital and Hospital Systems
EMS and hospital teams must follow a uniform PALS algorithm to minimize any confusion and duplication. They can also understand the assessment criteria, drug dosing standards, and communication formats through joint workshops and interdisciplinary drills. Sometimes, this may also involve working with electronic prehospital-to-hospital data transfer systems.
Invest in Pediatric-Specific Training and Equipment
The physiology, anatomy, and medication requirements of children differ significantly from those of adults. That is why you must ensure that prehospital providers can easily access pediatric-sized airway kits and other dosing charts. Conversely, all hospitals must verify that their pediatric crash carts are well-stocked and easily accessible.
Leveraging Technology Wisely
Early warning systems powered by artificial intelligence (AI) can be an excellent choice for hospitals. They can easily flag any deteriorating pediatric patient health. This also allows the timely activation of various PALS protocols in the long run. EMS agencies, on the other hand, can easily make use of remote consultation platforms to access pediatric specialists in real time.
Get PALS-certified for Better Hospital Outcomes!
The success of PALS lies in combining human skill, teamwork, and timely response. For EMS staff vs hospital teams, the differences in context should complement one another. EMS professionals bring unmatched adaptability, situational awareness, and rapid intervention skills to the table. Hospital teams, on the other hand, contribute advanced clinical expertise, coordinated support, and post-resuscitation care. The ideal pediatric emergency response system is one where both departments are aligned. Enroll in an online PALS certification from a recognized provider to ensure better outcomes. It will remain valid for 2 years and give you an edge over others when dealing with pediatric emergencies.
FAQs
1. What is covered in a PALS course?
A PALS course usually teaches you how to perform child and infant CPR with oxygen delivery and airway management techniques. You will also learn how an electrocardiogram (ECG) works and the importance of providing defibrillation or cardioversion.
2. How does PALS differ from BLS?
Unlike BLS, PALS is specifically not limited to cardiac arrest. Instead, the course includes a broader spectrum of pediatric medical emergencies, including but not limited to cardiac arrest, shock, or respiratory distress. The unique emotional and physiological needs of infants and children are usually central to PALS.
3. Is PALS harder than ACLS?
Both PALS and ACLS advanced courses, but the difficulty usually depends on your familiarity with pediatric care rather than with other adult cardiovascular emergencies. Both certifications also require an extensive understanding of advanced life support techniques.
PALS CERTIFICATION
Author
PALS Certification is a trusted provider of online life support training, offering PALS, BLS, and ACLS certification and renewal courses. Our flexible training programs follow industry guidelines, offer self-paced learning and instant certification, ensuring providers stay compliant, advance their credentials, and deliver high-quality patient care.