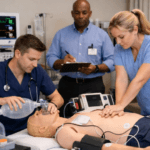
How to Identify Shock in Children?

Updated on: January 14, 2026
Shock in children happens when the body can’t get enough blood flow and oxygen to vital organs. It can result from severe fluid loss, infection, allergic reaction, or trauma. In the US, children with severe septic shock or sepsis face mortality rates between 9% to 18%. These rates can vary depending on factors such as the child’s overall health, the type of hospital, and the resources available for treatment. Identifying signs of shock in children can help prevent permanent organ damage and support faster, fuller recovery. Children often show fewer signs compared to adults because their bodies compensate longer than adults. However, if it happens, it might require immediate care. This guide will walk you through the ways to spot key signs of shock in children, different types, and ways to respond.
Read More: Children and chronic bronchitis: First aid and need for PALS Skills
What Is Shock in Children?
Shock in children occurs when circulation drops to a level where the body can’t keep organs supplied with enough oxygen. Pediatric shock is an acute energy failure. It occurs because of poor glucose or oxygen delivery. When the blood flow drops, the cells shift to anaerobic metabolism. Although not every child with shock will develop organ dysfunction, if the condition is not recognized and treated promptly, the risk of organ failure increases.
Children are difficult to assess because their bodies compensate better than adults’. They can also maintain near-normal blood pressure even when in shock. Due to such reasons, early recognition is difficult and critical. Shock is not just low blood pressure, but also poor perfusion. In children, the transition from compensated to uncompensated can occur very quickly.
Read More: PALS Post Arrest Shock Management Algorithm
What Are the Early Signs and Symptoms of Shock in Children?
Recognizing the signs of shock in children can save a child’s life. Here are some of the warning signs that caregivers and clinicians look for:
1. Changes in Behavior or Alertness
The first sign that you should watch out for is the sudden change in mood and behavior. The child might seem less responsive, confused, sleepy, or irritable. Babies might stop reacting to voices or smiling. All these early mental changes mean that the brain is not receiving enough oxygen.
2. Abnormal Vital Signs
Tachycardia in newborns refers to a resting heart rate that is naturally higher than that of older children. In contrast, adolescents are considered tachycardic when their resting heart rate rises above 100 beats per minute. If you are concerned that your child’s heart rate is unusually fast, it is important to seek advice from a healthcare professional.
3. Skin Changes and Poor Circulation
Check the child’s capillary refill and skin. If the skin looks clammy, cool, or pale, the circulation is poor. Another sign of poor circulation is when the feet and hands might feel cold, while the child’s body is warm. In several cases, particularly with septic shock, the skin might feel unusually flushed or warm early on.
4. Weak Pulse
When a child has a weak pulse, especially in the ankles or wrists, it means poor blood flow. In many cases, the pulse might be hard to find. This is a strong indicator that the organs are not getting enough blood.
5. Lower Urine Output
Children who urinate less than usual or go several hours without urinating might be in early shock. Low urine output indicates that the kidneys are not getting enough blood. This stands out as one of the most reliable early warning signs of shock in children.
6. Other Physical Signs
Watch out for cool legs and arms, hepatomegaly (swelling of the liver), rapid breathing, and bluish fingernails or lips. The lab tests might also show a high level of lactate, which leads to poor oxygen delivery to the body. These changes clearly show that the body is struggling to prevail and is switching to emergency mode.
What Are the Different Types of Shocks in Children?
Studies show that shock affects between 1.5% of children in general hospital settings and up to 44% of critically ill children. Additionally, the risk of death varies from about 4% to 33%, depending on the type and severity. Common causes include gastroenteritis, sepsis, malaria, and severe anemia, which often happen together. Knowing the type of shock is important because it helps decide the right treatment. Here’s a brief explanation of each of them:
Hypovolemic Shock
Hypovolemic shock occurs when a child loses too much body fluid or blood. It’s the most common type of shock in children and can develop quickly because children have a low volume of blood. Some of the most common causes of this shock include:
- Fluid shifts from diabetic ketoacidosis or burns
- Heavy bleeding from injury or surgery
- Severe dehydration due to vomiting or diarrhea.
Distributive Shock
This shock occurs when the blood vessels lose their tone, leading to uneven blood pooling and flow. Early signs might include warm feet and hands, but the organ perfusion declines. Common causes include:
-
Spinal cord injuries
- Severe allergic reactions (anaphylaxis)
- Sepsis (very common in the US
Cardiogenic Shock
Cardiogenic shock takes place when the heart cannot pump properly. This lowers the oxygen delivery to the body. Some of the main causes of this shock in children include:
- Excess fluid can worsen this sort of shock, which makes early detection essential.
- Myocarditis (viral infection affecting the heart)
- Severe congenital heart defects or arrhythmias
- Cardiomyopathy (heart muscle disease)
Obstructive Shock
Obstructive shock arises when blood flow is physically blocked, even if the heart is strong. Common causes include:
- Cardiac tamponade (fluid around the heart)
- Tension pneumothorax (air trapped in the chest)
- Pulmonary embolism (rare in children)
How to Respond if You Suspect Shock?
Apart from knowing the signs of shock in children, it’s also important to treat it as a medical emergency. Here’s what to do if you suspect shock:
For Caregivers and Bystanders:
- Call the emergency services immediately and take the child to the hospital.
- Lay the child down and, if it’s comfortable and doesn’t cause trouble breathing or pain, gently raise their legs.
- Keep the child warm with extra clothing or a blanket.
- Watch their basic signs, such as the color of the skin or lip, breathing, and responsiveness.
- Follow the ABC technique:
- Airway: Make sure the throat and mouth are clear.
- Breathing: Take a look to see if the child is breathing properly. If you’re trained, give rescue breaths when needed.
- Circulation: Look for signs of blood flow like pulse, normal skin color, and warmth.
- Don’t give the child antibiotics, fluids, or medicine in large amounts at home.
Hospital Treatment (for Medical Staff Only):
- Monitor the urine output, heart rate, respiratory rate, capillary refill, and blood pressure.
- Begin the fluid resuscitation fit for the suspected type of shock. For the hypovolemic/distributive: isotonic crystalloid boluses (10 to 20 mL/kg, reprises as needed up to 40 to 60 mL/kg in the hour), until the cause is cardiogenic.
- Treat the underlying cause, for instance, treating septic shock with antibiotics.
- Escalate care to the Pediatric Intensive Care Unit (PICU) if required for worsening or severe shock.
Read More: Basic Airway Management in Children
How to Prevent Shock in Children?
Preventing shock in children begins with early action by healthcare workers, caregivers, and parents, and awareness. Some of the main steps include:
- Treat the Infections Early: Address coughs, fevers, and wounds immediately. Keep the vaccinations up-to-date, including the flu and pneumococcal shots. Excellent hygiene and early detection lower the risks of sepsis, which accounts for about 22% of child deaths in the US.
- Keep Children Hydrated: Provide more fluids, especially during the hot weather or illness. Seek medical help if the child cannot keep fluids down, has dehydration, stops urinating, or becomes weak.
- Manage Allergies Safely: Children with severe allergies are at a much higher risk of anaphylactic shock. Make sure to carry prescribed epinephrine, inform the caregivers and schools, and know the triggers. Immediate treatment can help prevent shock.
- Prevent Trauma: Ensure a safe setting and teach safety rules, such as seatbelts and helmets. For injuries with heavy bleeding, apply pressure and then seek emergency care without any delay.
Enroll Today to Learn Life-Saving Action in Pediatric Shock!
Shock in children can become life-threatening very quickly. When you notice the early signs, you must act immediately. Getting medical help quickly and identifying the symptoms early can prevent severe issues and might even save a child’s life. If you care for or work with children, it’s critical to know how to respond during a crisis. Taking the Pediatric Advanced Life Support (PALS) program gives you the skills to remain calm and take the correct steps when every second counts. Your confident and instant actions make all the difference, helping a child survive and then recover safely.
FAQs
1. Can a child be in shock even if the skin feels warm?
Yes. In distributive shock, the blood vessels become wide, making the skin warm even when the organs lack proper blood flow.
2. How fast should fluids be given to a child in shock?
Give 10 to 20 mL/kg of isotonic fluids immediately, and then reassess after every round.
3. When should a child be moved to intensive care?
If the child stays confused, weak, or has low urine output, despite treatment, move them to the PICU without any delay.
PALS CERTIFICATION
Author
PALS Certification is a trusted provider of online life support training, offering PALS, BLS, and ACLS certification and renewal courses. Our flexible training programs follow industry guidelines, offer self-paced learning and instant certification, ensuring providers stay compliant, advance their credentials, and deliver high-quality patient care.