- 4.0 CE Credit Hours
- For Pediatric Responders
- Includes Videos, Megacode Scenarios, Practice Tests & More
- FREE BLS Included
$119.00 $169.00
Get CertificateThe ACLS tachycardia algorithm functions as a structured guide and provides healthcare providers with a systematic approach to handling patients experiencing a heart rate exceeding 150 beats per minute. This algorithm is ideal for adults and ensures a strategic response to tachycardia, emphasizing the need for precise interventions to optimize medical outcomes.
It enables healthcare professionals to navigate through the algorithm when confronted with an adult patient exhibiting tachycardia. These procedural steps ensure adequate perfusion and initiate synchronized cardioversion while administering antiarrhythmic medications. This facilitates timely interventions and enhances patient outcomes. Here is the step-by-step flowchart for the ACLS tachycardia algorithm.

$119

$119.00 $169.00
Get Certificate$119.00 $169.00
Get Certificate$36.95 $39.90
Get Certificate
An ACLS Bradycardia algorithm helps you learn the guiding interventions for emergency slow heart rates
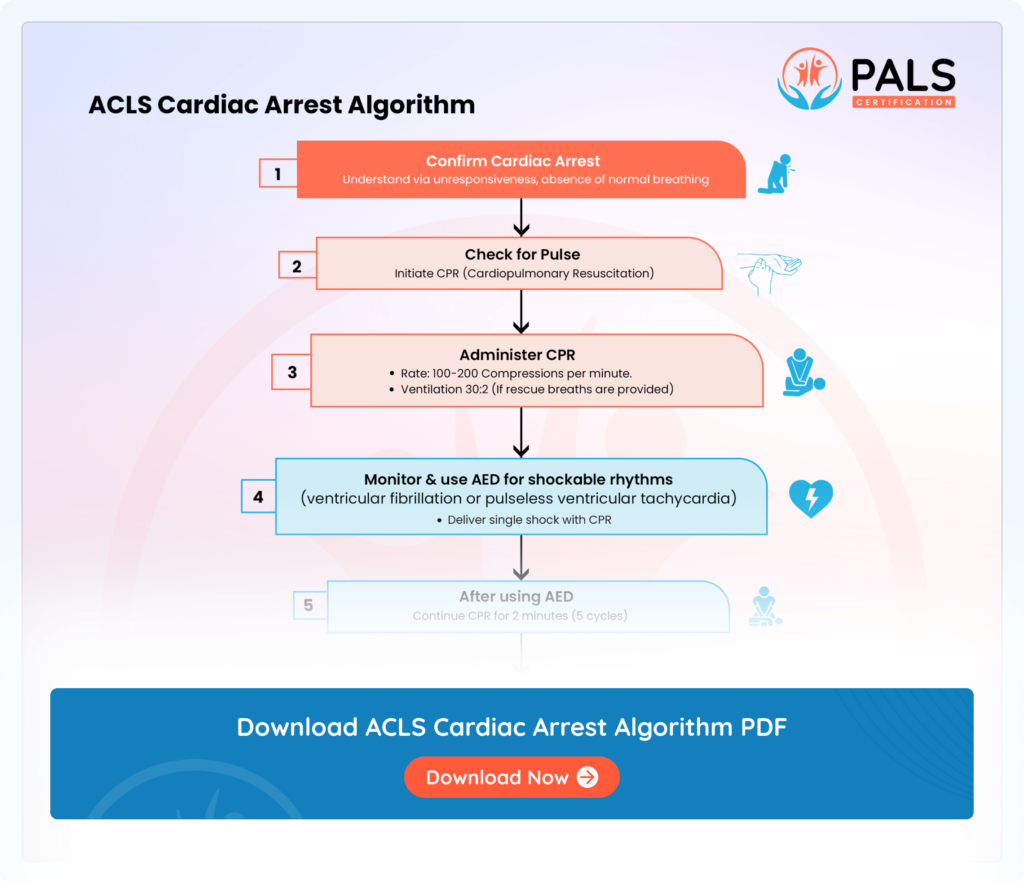
The ACLS cardiac arrest algorithm directs resuscitation efforts, outlining steps like patient assessment, CPR initiation, defibrillation if needed, medication administration, reversible cause evaluation, and advanced interventions.
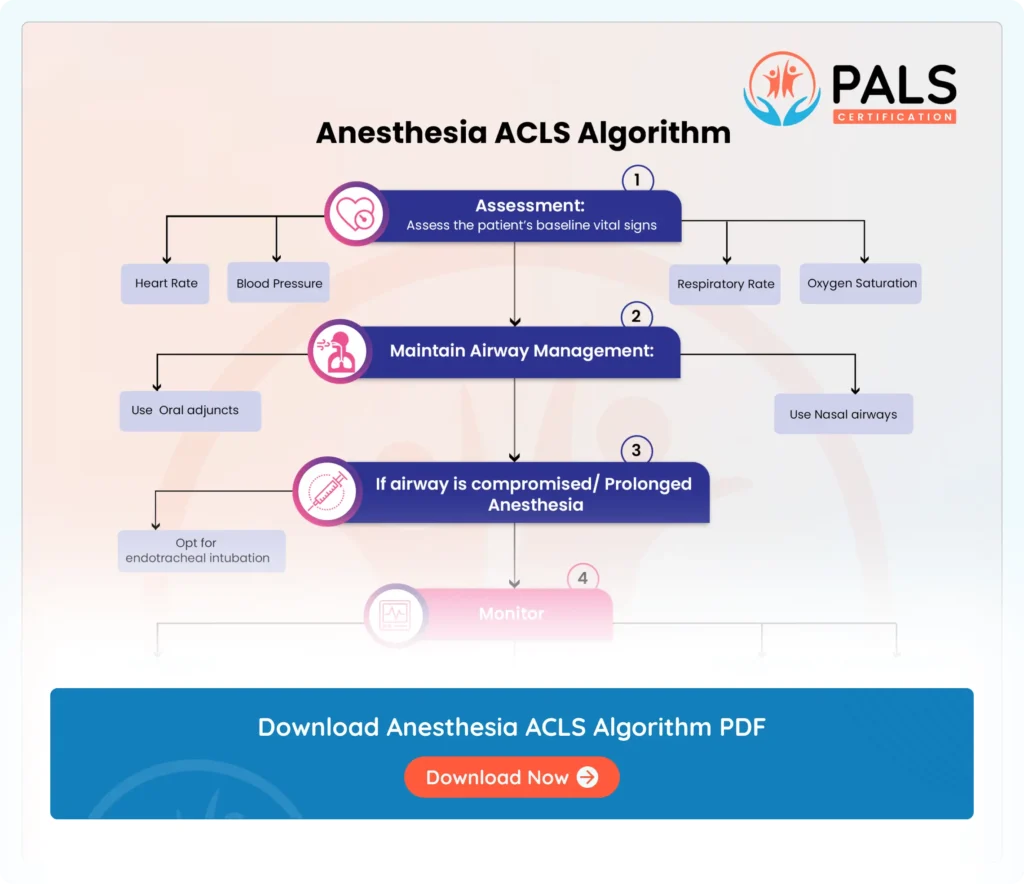
Know how to assess vital signs, secure airway and initiate CPR when needed. Administer ACLS drugs, address reversible causes and adapt management to patient’s condition for anesthesia emergencies.