Advanced Airway CPR and Bag Mask Ventilation: A Thorough Guide
Updated on: March 4, 2026
Effective resuscitation in emergencies often depends on maintaining oxygen flow to the brain and vital organs. Advanced airway management and bag-mask ventilation (BMV) are critical techniques for healthcare providers responding to cardiac arrest or respiratory failure. While basic cardiopulmonary resuscitation (CPR) keeps blood moving, adding advanced airway skills allows continuous chest compressions and controlled ventilation, improving chances of survival. Proper BMV ensures oxygen delivery when the patient cannot breathe independently, while advanced airway devices secure the airway for prolonged support.
This guide will explore what CPR with an advanced airway means, how CPR is different with advanced airway, and how to perform it safely using effective bag-mask ventilation techniques.
Read More: Basic Airway Management in Children
What is CPR With an Advanced Airway?
When rescuers place an advanced airway (such as an endotracheal tube or supraglottic device) during CPR, it becomes easier to give chest compressions without pausing for breaths. According to the American Heart Association (AHA) 2020/2024 guidelines, once the airway is secured, the team delivers one breath every six seconds (≈10 breaths per minute in adults) while compressions proceed uninterrupted.
- Advantages: Continuous circulation, improved oxygen delivery, fewer interruptions.
- Important caveats: Advanced airway placement should not delay chest compressions or defibrillation.
In children and infants, the ventilation rate changes slightly (20-30 breaths/min in some cases when an advanced airway is in place) but the principle remains: secure airway, minimize breaks, ventilate at a defined rate.
Which Advanced Airway Devices Are Used in CPR?
During CPR, healthcare providers may insert special airway devices to keep the breathing passage open and deliver oxygen more effectively. These advanced airway devices help maintain ventilation without interrupting chest compressions in both adults and children. The common types of devices used for CPR with an advanced airway are as follows:
ETT (Endotracheal Tube)
The ETT (Endotracheal Tube) is a cuffed tube that is directly inserted into the trachea via the nose or mouth. It offers the safest airway and allows accurate control of oxygen delivery and ventilation. The cuff seals the trachea and prevents air leakage. This helps lower the chances of aspiration (fluids entering the lungs).
SGA (Supraglottic Airway)
This device sits right above the glottis (the vocal cords) instead of entering the trachea. Some of its common examples are LMA (laryngeal mask airway) and i-gel. SGA is much easier and quicker to insert than ETT. This makes it helpful when immediate airway management is needed. However, they might not offer protection against aspirations as effectively as the ETTs. This is perfect for providers who have basic to intermediate airway skills. It’s also ideal for situations where the incubation is delayed or difficult.
Cricothyroidotomy (Surgical Airway)
These CPRs with advanced airway devices are also known as “surgical airway”. It’s used only during extreme emergencies when every airway technique fails. In this procedure, an opening is made via the cricothyroid membrane to insert the breathing tube directly into the trachea. Since this is a last-resort method, it’s conducted by experienced medical professionals under critical conditions.
Read More: AED vs CPR: Know When and How to Use in Emergencies
When Do You Use the Advanced Airway Devices?
The CPR with and Advanced Airway devices are used when basic airway techniques, like head tilt–chin lift, jaw thrust, or bag-mask ventilation, do not provide effective oxygenation or ventilation. Their use depends on the patient’s condition, response to initial resuscitation, and the rescuer’s skill level.
You typically use an advanced airway when:
- Bag-mask ventilation is inadequate or difficult to maintain.
- The patient shows persistent low oxygen levels despite effective compressions and ventilation.
- There is a need for definitive airway protection to prevent aspiration of fluids, vomit, or blood.
- The rescuer wants to provide continuous chest compression without pausing for breaths.
- The situation demands precise control of ventilation and oxygen delivery, such as during prolonged resuscitation or transport.
In emergency and cardiac arrest settings, the choice of the advanced airway CPR device used will depend on the rescuer’s expertise, available equipment, and patient condition. Advanced airways ensure that oxygen and carbon dioxide exchange continues effectively while keeping the airway protected and allowing compressions to continue without interruption.
Read More: Basic Airway Management in Children
Performing Continuous Chest Compressions the Right Way
In basic CPR, a normal cycle includes 30 chest compressions followed by 2 rescue breaths. Once an advanced airway (like an endotracheal tube or supraglottic device) is in place, compressions are performed continuously without pausing for breaths. Here’s how to do it correctly:
- Compression Rate: Maintain 100–120 compressions per minute, roughly matching the rhythm of “Stayin’ Alive” by the Bee Gees or similar-tempo songs.
- Compression Depth:
- Adults: about 2 inches (5–6 cm)
- Children: about 2 inches (5 cm)
- Infants: about 1½ inches (4 cm)
- Allow Full Chest Recoil: After each compression, let the chest return fully to its normal position. Don’t lean on the chest between compressions.
- Minimize Interruptions: Stop compressions only for essential tasks, such as defibrillation (using an AED), rhythm checks, or critical interventions.
- Rescuer Rotation: If two rescuers are present, switch every 2 minutes (or sooner if fatigued) to maintain effective depth and rate.
- Ventilation With an Advanced Airway: Deliver 1 breath every 6 seconds (about 8–10 breaths per minute) asynchronously, meaning breaths continue while compressions remain uninterrupted.
- Avoid Over-Ventilation: Give each breath over 1 second, just enough to make the chest rise gently.
Read More: One and Two Rescuer BLS for Infants (0 to 12 Months)
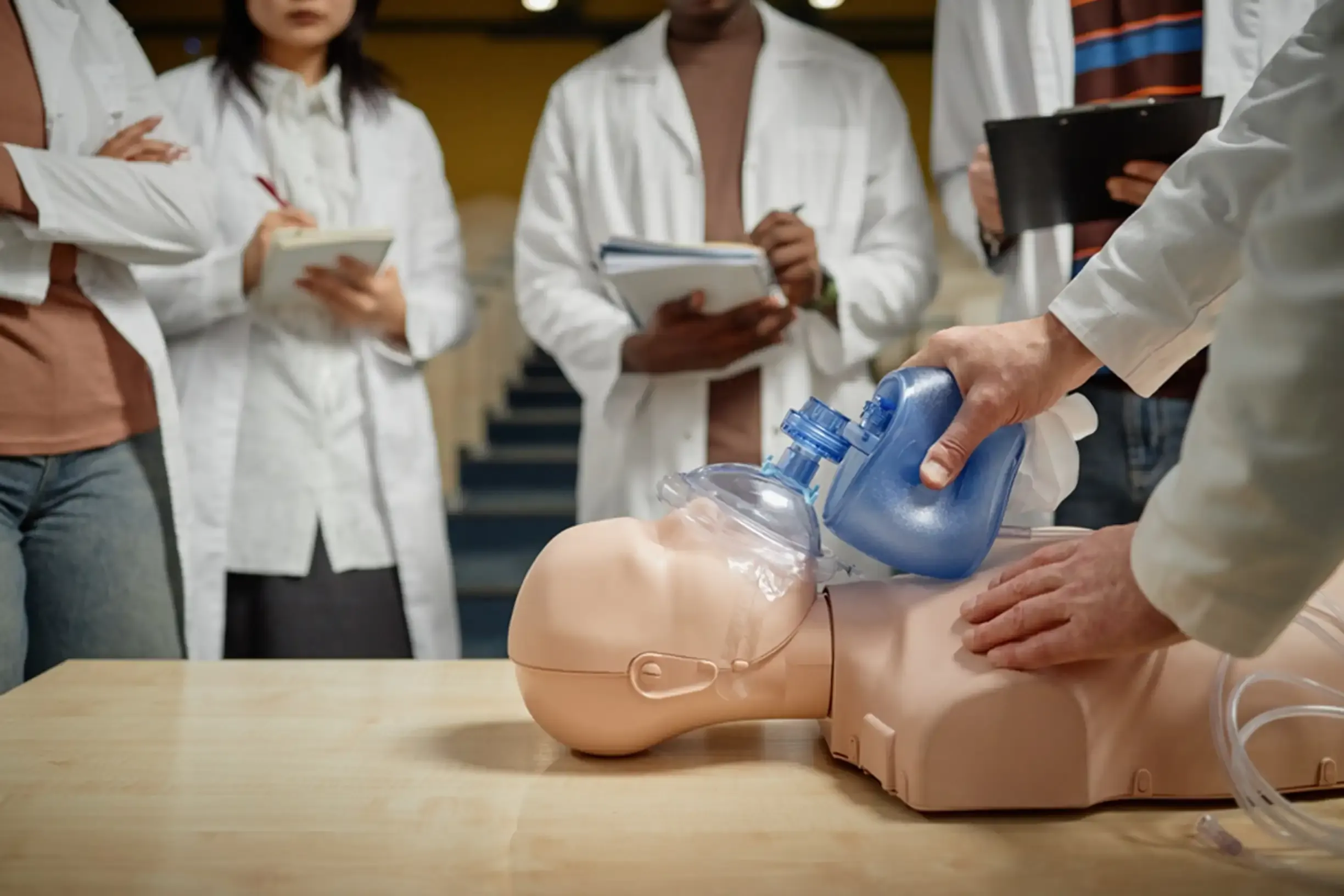
What is Bag-Mask Ventilation During CPR?
The CPR bag mask device is used during and before the advanced airway placement. It helps in delivering oxygen until a proper airway is in place. Knowing how to use it properly and when to switch to an advanced airway is essential for effective CPR.
Before the Advanced Airway Is Placed
- Use the bag-valve-mask (BVM) to give rescue breaths after every 30 compressions.
- If two trained rescuers are present, you can give 10 breaths per minute asynchronously (without pausing compressions).
- Make sure the mask seals tightly around the face to prevent air leaks.
- Watch for visible chest rise with each breath to confirm air entry.
- Avoid excessive air pressure to reduce the risk of stomach inflation and regurgitation.
Transitioning to an Advanced Airway
- Keep performing compressions while preparing to place the airway.
- Limit pauses, quick transitions prevent oxygen loss.
- Many protocols recommend delaying airway placement until after two CPR cycles if bag-mask ventilation is maintaining oxygen levels well.
- Once ready, the rescuer continues BVM ventilation until the airway device is secured.
After the Advanced Airway Is Placed
- Provide continuous compressions at 100–120 per minute.
- Deliver one breath every 6 seconds (about 8–10 per minute) through the airway device.
- Use a two-handed technique to keep a firm seal and reduce leaks.
- Each breath should last one second, just enough to make the chest rise.
- Avoid overinflation, too much air can raise chest pressure and lower blood flow to the heart.
Monitoring and Adjustments
- Trained providers use capnography (EtCO₂) to confirm proper ventilation and circulation.
- If using a mechanical ventilator, adjust the settings to match the compression phase. This helps maintain consistent pressure and oxygen delivery.
- Stay alert for any drop in chest rise, color change, or low EtCO₂ levels. These can signal poor ventilation or loss of airway seal.
Master Continuous Compression and Advanced Airway Techniques!
When you perform CPR with an advanced airway, continuous chest compressions and asynchronous bag breaths, it will keep the oxygen and blood flowing during cardiac arrest. The success depends heavily on careful monitoring, proper method, controlled ventilation and smooth transitions. Many studies show promise, but it also has risks if the airway placement leads to hyperventilation or delays.
You might be familiar with the basic CPR techniques. However, if you want to learn advanced airway methods and transitions, take up our BLS Course today. It’s created for rescuers and clinicians who want to go way beyond the theory and gain confidence in high-stakes airway management during CPR.
FAQs
What is the difference between basic CPR and CPR with an advanced airway?
The rescue breathing with advanced airway allows continuous chest compressions without pausing for breaths. Basic CPR follows 30 compressions and 2 breaths. An advanced airway also improves ventilation control and lowers aspiration risk.
When should an advanced airway be placed?
Use the rescue breaths with advanced airway when bag-mask ventilation is inadequate, during prolonged resuscitation, or when continuous compressions are needed. Some protocols delay placement until after two compression cycles if ventilation is effective.
How do compressions affect ventilation and EtCO2?
Continuous compressions can lower the tidal volumes and cause oscillation artifacts on EtCO₂ readings. Deliver ventilations asynchronously at about 8 to 10 breaths per minute while compressions continue.
How often should rescuers rotate?
You rotate rescuers every 2 minutes to prevent fatigue. Interruptions should only take place for critical tasks such as defibrillation, rhythm checks, or airway placement.
PALS CERTIFICATION
Author
PALS Certification is a trusted provider of online life support training, offering PALS, BLS, and ACLS certification and renewal courses. Our flexible training programs follow industry guidelines, offer self-paced learning and instant certification, ensuring providers stay compliant, advance their credentials, and deliver high-quality patient care.